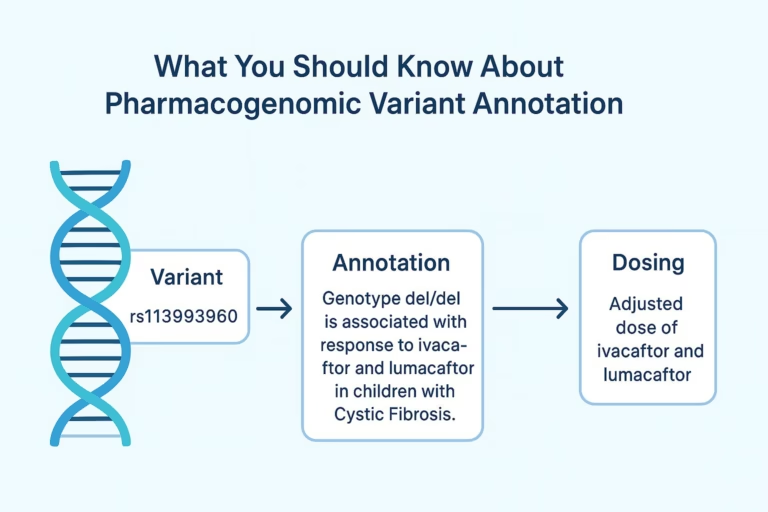
The UK has taken a major step forward in precision prescribing with the publication of its first national pharmacogenomic guideline, focused on the antiplatelet drug clopidogrel. Developed by the UK Centre of Excellence in Regulatory Science and Innovation in Pharmacogenomics (UK CERSI-PGx)—led by the University of Liverpool—this guideline brings the UK closer to embedding genetic testing into routine clinical practice.
Clopidogrel is widely prescribed across the NHS to prevent blood clots in patients with coronary artery disease, cerebrovascular disease, and peripheral arterial disease. But while the medication is standard therapy, its effectiveness varies substantially between individuals. The new guideline directly addresses this variability by recommending CYP2C19 genotyping for patients before clopidogrel therapy is initiated.
Clopidogrel and CYP2C19
Clopidogrel is a prodrug—meaning it must be metabolised by the liver to convert it into its active form. This activation process depends heavily on a liver enzyme called CYP2C19. Genetic variations in the CYP2C19 gene determine how much of this enzyme an individual produces, influencing how well they convert clopidogrel into its active compound.
Patients with certain CYP2C19 variants—known as loss-of-function alleles—produce lower levels of the enzyme. Because of this, they activate clopidogrel less efficiently, reducing the drug’s ability to prevent clotting. This reduced response can lead to poorer clinical outcomes, including increased risk of heart attack or stroke.
The prevalence of these variants is significant:
- 20–30% of individuals of European ancestry carry reduced-function CYP2C19 alleles
- 50–60% of individuals of Asian descent carry these variants
Given these numbers, the guideline makes the case that CYP2C19 testing is not a niche intervention—it is relevant to a substantial proportion of the UK population.
A UK-Specific, Clinically Focused Guideline
Several international bodies, including CPIC (Clinical Pharmacogenetics Implementation Consortium) and DPWG (Dutch Pharmacogenetics Working Group), already provide evidence-based recommendations for clopidogrel dosing based on CYP2C19 genotype. However, the new UK guideline was designed with a different emphasis.
Rather than replicating international guidance, UK CERSI-PGx aimed to create practical, clinically applicable recommendations tailored to NHS care pathways. The guideline provides detailed direction on:
- Eligibility for testing
- How pharmacogenomic testing should be integrated into existing clinical workflows
- Which genetic variants should be included in CYP2C19 assays
- Expected turnaround times for results
- Recommended actions based on a patient’s genotype
- Health-economic implications and cost-effectiveness data
Professor Sir Munir Pirmohamed, Centre Lead at the University of Liverpool, highlighted the significance of the guideline, stating that the goal is to ensure patients receive “the right treatment at the right dose, based on their genetics.” Integrating CYP2C19 testing into routine pathways can improve drug effectiveness, reduce preventable adverse reactions, decrease healthcare costs, and ease pressure on the NHS by preventing avoidable complications.
Professor Dame Sue Hill, Chief Scientific Officer for England, emphasised that the guideline is “an important step in using genomics to inform treatment pathways and prevent avoidable side effects.” She also noted that the inclusive and multidisciplinary approach used here will guide future UK pharmacogenomic guidelines.
From a regulatory perspective, MHRA Chief Safety Officer Dr Alison Cave described pharmacogenomics as a “gamechanger for patient safety and wellbeing,” highlighting how genetic insights can help clinicians select the right therapy for each patient—minimising risk and maximizing therapeutic benefit.
Conclusion
This is the first in a series of pharmacogenomic guidelines planned by UK CERSI-PGx, and its release marks the beginning of a more systematic integration of genetics into prescribing practice. With clopidogrel among the most commonly prescribed antiplatelet drugs in the UK, implementing CYP2C19 testing at scale has the potential to significantly improve cardiovascular outcomes nationwide.
The guideline and its accompanying editorial were published on 4 December 2025 in the British Journal of Clinical Pharmacology, marking a milestone for UK regulatory science and precision medicine.
As more guidelines emerge, the NHS is positioned to become a global leader in the clinical application of pharmacogenomics—ensuring future prescribing is safer, smarter, and more personalized than ever before.